

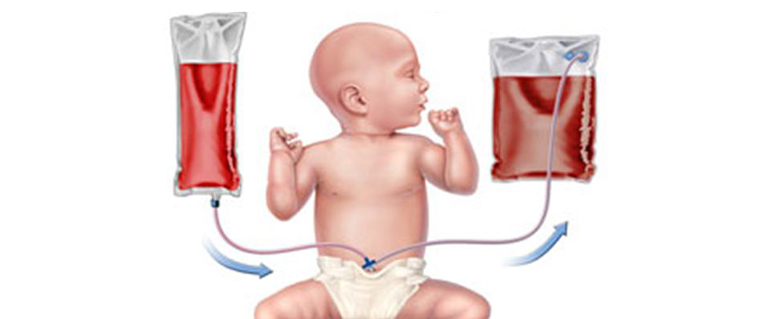
The process of exchanging blood between two donors is called a transfusion exchange. This process is used in the case of neonatal patients, who may need the additional oxygen-carrying capacity provided by the donor's red cells and plasma. Exchange transfusion can be used in other situations as well, such as when one person has donated blood for someone else and needs to receive it back again.
A blood transfusion is an injection of one or more units of blood into a vein by intravenous, intra-arterial, or deep intravascular administration to increase the blood volume in patients who are experiencing hypovolemia (low blood volume) or anemia. Blood transfusions may also be given as part of some types of chemotherapy. The World Health Organization estimates that a minimum 2.3 million units (approximately 17 kg) of packed red cells must be transfused per year for surgical care alone.
Expectant mothers and neonates who are undergoing a blood transfusion exchange should be prepared for some changes in their body. Pregnant women are at risk of iron deficiency, anemia, and thrombocytopenia. These conditions can be prevented by getting a blood transfusion exchange. Blood transfusions are often used to treat iron deficiency, anemia, and thrombocytopenia in pregnant women and neonates. However, there may be some side effects such as low hemoglobin levels and low platelet counts that need to be monitored very closely.
Neonatal blood transfusions are a life-saving procedure, but they can pose risks. The most common problems that can result from neonatal exchange are incompatibility and infection. Incompatibility is a risk of the first day of life for some infants, where the blood type or Rh factor of the infant does not match the mother’s. Infection is a risk when an exchange occurs when an infant has been exposed to any infectious disease in utero or at birth.
Neonatal exchange is a procedure in which two neonates with incompatible blood types are exchanged at birth to prevent all immunization from maternal antibodies, which can lead to hemolytic disease of the newborn (HDN). and other complications. Neonatal blood transfusions are a life-saving procedure, but they can pose risks. The most common problems that can result from neonatal exchange are incompatibility and infection. Incompatibility is a risk of the first day of life for some infants, where the blood type or Rh factor of the infant does not match the mother’s.
- Neonatal hyperbilirubinemia is one of the most common causes of morbidity and mortality in newborns. It is a condition that results in jaundice, which can be severe enough to cause brain damage. Exchange transfusion for neonatal hyperbilirubinemia is a treatment option for newborns with severe jaundice. It involves replacing the blood of an infant with a blood product that contains more bilirubin-binding protein than the infant's own blood. Exchange transfusion has been used to treat neonatal hyperbilirubinemia since the 1980s and how it has evolved over time. Exchange transfusion may be used in other conditions such as hydrocephalus and encephalopathy associated with cerebral palsy or traumatic brain injury.
Neonatal hyperbilirubinemia is jaundice found in infants less than 28 days old. Newborns are often jaundiced because their first bowel movements have bilirubin-rich feces, which can pass through the newborn's intestine and into the bloodstream. Jaundice can also be caused by liver disease, blood conditions, or a defective enzyme called bilirubin glucuronidase. Exchange transfusion is a treatment option for neonatal hyperbilirubinemia that involves replacing an infant's blood with a blood product that contains more bilirubin.
There are three types of blood transfusions:whole blood transfusion, red blood cell transfusion, and platelet transfusion.
A whole blood transfusion involves a single unit of blood, which is drawn from an individual and given to another person. It is the most common type of transfusion because it can be safely and effectively given through intravenous, intramuscular or intraosseous injection. The donor usually receives a minor amount of red blood cells back in the process. The red blood cell transfusion involves collecting a unit of red cells (from a donor or from one's own body) that are then separated into its component parts and syringed into the recipient. This form is used when someone needs more than two units of red cells, or when they need the blood to be given through a different route.
Platelet transfusion is generally not used for survival purposes but is sometimes used in conjunction with other treatments. Many people find that donating blood can be quite satisfying and give a person some peace of mind because it helps reduce the number of patients on waiting lists. In fact, donating may provide more benefits than simply meeting patient needs for blood components for transfusions.